Bile’s Role in Thyroid Health
If you’re battling thyroid symptoms like fatigue or weight issues from Hashimoto’s or Graves’, bile might be your unsung hero. As a certified nutrition specialist and licensed nutritionist, I’m here to explain how bile supports digestion and your thyroid. Let’s explore how it works and simple ways to boost bile flow for a vibrant thyroid, based on nutritional therapy principles.
What Is Bile?
Bile, produced by your liver and stored in your gallbladder, is a fluid that helps digest fats in your small intestine. It breaks fats into fatty acids, which carry fat-soluble vitamins (D, A, K, E) to support your thyroid. Bile also removes toxins, reducing inflammation that can stress your thyroid.
Bile and Thyroid Function
Your thyroid needs vitamins like D for hormone production and immune health, especially in autoimmune conditions. Poor bile flow, often from low fat intake or gallbladder issues, can limit these vitamins, worsening symptoms like brain fog or joint pain. Bile also detoxifies hormones like estrogen, which can disrupt thyroid function if imbalanced.
Bile and Detoxification
Bile binds toxins in your intestines for removal through stool. Sluggish bile flow traps toxins, increasing inflammation and thyroid stress. For example, trapped toxins might raise estrogen, interfering with thyroid hormones.
Common Bile Issues
Factors like low-fat diets, stress, or gallbladder problems can reduce bile flow, causing:
Fat Malabsorption: Limits vitamin D, worsening thyroid symptoms.
Toxin Buildup: Increases inflammation.
Digestive Discomfort: Like bloating after fatty meals.
These can make you feel sluggish and affect thyroid health.
Practical Tips for Thyroid-Friendly Bile Flow
Here are easy ways to support bile and your thyroid, fitting your love for home-cooked meals:
Eat Healthy Fats: Include avocado or olive oil to stimulate bile release.
Support Liver Health: Try beets or leafy greens to boost bile production.
Reduce Stress: Take 5 deep breaths before meals to support digestion.
Stay Hydrated: Drink 8 glasses of water daily to aid bile flow.
Limit Processed Foods: Swap fried foods for whole fats.
Try Supplements: Bile salts or ox bile can help. Visit www.outofthewoodsnutrition.com/dispensary, but consult your doctor.
Why It Helps
Healthy bile flow delivers vitamins to your thyroid, reduces inflammation, and supports detox, easing symptoms like fatigue.
Work With Your Doctor
I don’t diagnose, but I can guide you with diet and lifestyle. Work with me or your healthcare provider to monitor thyroid levels and discuss symptoms like bloating.
Take Action
Try adding avocado to a meal this week. Book a consultation at www.outofthewoodsnutrition.com. Visit www.outofthewoodsnutrition.com/dispensary. Reply for a custom tip!
What’s your favorite healthy fat? Comment below!
About the Author: I’m a certified nutrition specialist and licensed nutritionist, helping women with thyroid conditions feel vibrant. Visit www.outofthewoodsnutrition.com for more tips.
Stomach Acid’s Role in Thyroid Health
If you’re dealing with thyroid issues like Hashimoto’s or Graves’, you might feel sluggish or struggle with hair loss. As a certified nutrition specialist and licensed nutritionist, I’m here to share a hidden hero: stomach acid. This powerhouse helps digest food and deliver nutrients to your thyroid. Let’s explore how stomach acid works and simple ways to support it for a vibrant thyroid, based on nutritional therapy principles.
Why Stomach Acid Matters
Your stomach produces hydrochloric acid (HCl) to break down food, especially proteins, into nutrients like iodine and amino acids that your thyroid needs for hormone production. HCl also kills harmful bacteria and protects your gut. Low stomach acid, common in thyroid conditions, can limit nutrient absorption, worsening symptoms like fatigue or brain fog.
How Stomach Acid Supports Your Thyroid
HCl activates pepsin, an enzyme that digests proteins into amino acids, which are building blocks for thyroid hormones like T3 and T4. It also frees minerals like iodine and selenium from food. Without enough HCl, your thyroid might miss these nutrients, leading to increased inflammation or autoimmune flares.
Common Causes of Low Stomach Acid
Factors that reduce stomach acid include:
Stress: Triggers “fight or flight” mode, slowing acid production.
Aging: Acid levels naturally decline with age.
Medications: Antacids can lower HCl, reducing nutrient absorption.
Low HCl can cause bloating, reflux, or nutrient deficiencies, all impacting your thyroid.
Stomach Acid and Inflammation
Low stomach acid can lead to undigested food in your gut, causing inflammation or leaky gut. This stresses your thyroid, especially in autoimmune conditions like Hashimoto’s, worsening symptoms like joint pain.
Practical Tips for Thyroid-Friendly Stomach Acid
Here are easy ways to support stomach acid and your thyroid, perfect for home-cooked meals:
Chew Slowly: Take 20-30 seconds per bite to signal acid production.
Eat Protein-Rich Foods: Try chicken or fish to stimulate HCl.
Reduce Stress: Take 5 deep breaths before meals to activate your vagus nerve.
Avoid Overeating: Smaller meals are easier to digest.
Stay Hydrated: Drink water between meals to support digestion.
Try Supplements: Betaine HCl or apple cider vinegar can aid acid levels. Visit www.outofthewoodsnutrition.com/dispensary, but consult your doctor, especially with thyroid meds. I can help you figure out just what dose you need.
Why It Helps
Healthy stomach acid ensures your thyroid gets nutrients, reduces inflammation, and supports gut health, easing symptoms like fatigue or mood swings.
Work With Your Doctor
I don’t diagnose, but I can guide you with diet and lifestyle. Work with your healthcare provider to monitor thyroid levels and discuss symptoms like reflux to explore stomach acid’s role.
Take Action
Try chewing slowly or eating a protein-rich meal this week. Book a consultation at www.outofthewoodsnutrition.com. Visit www.outofthewoodsnutrition.com/dispensary.
What’s your favorite protein-rich meal? Comment below!
About the Author: I’m a certified nutrition specialist and licensed nutritionist, helping women with thyroid conditions feel vibrant. Visit www.outofthewoodsnutrition.com for more tips.
How Digestive Enzymes Support Your Thyroid
If you’re navigating thyroid challenges like Hashimoto’s or Graves’ disease, you might feel tired, foggy, or struggle with weight. As a certified nutrition specialist and licensed nutritionist, I’m here to share a key player in thyroid health: digestive enzymes. These tiny helpers break down food to fuel your thyroid with nutrients. Let’s explore how enzymes work and simple ways to support them for a vibrant thyroid, based on nutritional therapy principles.
What Are Digestive Enzymes?
Digestive enzymes are proteins that break down carbs, proteins, and fats into smaller pieces your body can absorb. Your thyroid needs these nutrients—like iodine, selenium, and zinc—to produce hormones that keep you energized. Enzymes work in your mouth, stomach, and small intestine, ensuring your thyroid gets what it needs. Without enough enzymes, digestion slows, starving your thyroid and worsening symptoms like fatigue.
Key Enzymes for Thyroid Health
Amylase: Found in saliva and pancreatic juices, it breaks carbs into sugars for thyroid energy.
Pepsin: In the stomach, it digests proteins into amino acids for thyroid hormone production.
Lipase: In the small intestine, it breaks fats into fatty acids, carrying vitamins like D for thyroid support.
Low enzyme activity, often from stress or poor diet, can limit nutrient absorption, increasing thyroid stress.
Enzymes and Inflammation
Poor enzyme function can lead to undigested food in your gut, causing inflammation. This is like a fire in your body, worsening autoimmune thyroid symptoms like joint pain or brain fog. For example, low pepsin might reduce amino acid absorption, impacting thyroid hormone production. Supporting enzymes calms this inflammation.
Common Enzyme Issues
Factors like stress, low stomach acid, or processed foods can reduce enzyme activity, leading to:
Bloating: Undigested food ferments in your gut.
Nutrient Deficiencies: Starves your thyroid of selenium or zinc.
Leaky Gut: Triggers inflammation, worsening Hashimoto’s flares.
These issues can make you feel sluggish and affect thyroid function.
Practical Tips for Thyroid-Friendly Enzyme Support
Here are easy ways to boost enzymes and thyroid health, perfect for home-cooked meals:
Chew Thoroughly: Take 20-30 seconds per bite to activate salivary amylase.
Eat Enzyme-Rich Foods: Try pineapple (bromelain) or papaya (papain) to aid digestion.
Reduce Stress: Take 5 deep breaths before meals to support enzyme production.
Limit Processed Foods: Swap chips for whole foods like veggies to reduce gut stress.
Stay Hydrated: Drink 8 glasses of water daily to support enzyme function.
Try Supplements: Digestive enzymes or betaine HCl can help. Visit www.outofthewoodsnutrition.com/dispensary, but consult your doctor, especially with thyroid meds.
Why It Helps
Healthy enzyme activity ensures your thyroid gets nutrients, reduces inflammation, and supports your gut microbiome, easing symptoms like fatigue or mood swings.
Work With Your Doctor
I don’t diagnose or treat conditions, but I can guide you with diet and lifestyle. Work with your healthcare provider to monitor thyroid levels and discuss symptoms like bloating to explore enzyme support.
Take Action
Try chewing slowly or adding pineapple to a meal this week. Book a consultation at www.outofthewoodsnutrition.com for a personalized plan. Visit www.outofthewoodsnutrition.com/dispensary for supplements. Reply to my newsletter for a custom tip!
What’s your favorite enzyme-rich food? Comment below and let’s chat!
About the Author: I’m a certified nutrition specialist and licensed nutritionist, passionate about helping women with thyroid conditions feel vibrant using functional medicine and simple strategies. Visit www.outofthewoodsnutrition.com for more thyroid health tips.
6 Common Reasons Your Thyroid Symptoms Fluctuate
It's common for thyroid patients to feel frustrated when symptoms like fatigue, brain fog, hair loss, weight changes, mood swings, joint pain, or temperature intolerance seem to come and go, worsen, or shift without clear reason.
From a functional medicine/root cause perspective, fluctuating symptoms are often a sign that the body is dynamically responding to underlying imbalances — not just a static "thyroid problem."
Functional medicine views the thyroid as part of an interconnected system (hormones, immune system, gut, adrenals, detoxification pathways, and more), and symptoms change because these root causes are rarely fixed in one state.
6 common reasons your thyroid symptoms fluctuate:
1. Autoimmune Flares (Especially in Hashimoto's or Graves')
In autoimmune thyroid conditions like Hashimoto's thyroiditis (the leading cause of hypothyroidism) or Graves' disease (hyperthyroidism), the immune system mistakenly attacks the thyroid gland. This isn't a constant attack but occurs in waves or "flares."
In Hashimoto's, antibodies such as thyroid peroxidase antibodies (TPOAb) and thyroglobulin antibodies (TgAb) target key thyroid enzymes and proteins. During a flare, Th1 or Th17 immune pathways activate, leading to inflammation and thyroid cell destruction. This can cause an unpredictable and inconsistent release of stored thyroid hormones giving you temporary hyperthyroid-like symptoms such as anxiety or palpitations before swinging back to more hypothyroid symptoms as tissue is lost from the destruction.
Some common triggers for this happening are: Stress which elevates cortisol causing a shift in immune system balance, viral or bacterial infections which cause issues via molecular mimicry— Epstein-Barr virus along with gluten proteins resemble thyroid tissue, seasonal changes, poor sleep, or inflammatory foods.
Molecular mimicry causes your immune system to attack your thyroid.
Why symptoms change: Flares can last days to weeks, with antibody levels spiking and dropping, creating unpredictable symptom intensity.
What to do about it: Test antibody levels repeatedly because they do fluctuate-it’s nice to have a baseline level you can measure against, identify food triggers with an elimination diet or at a minimum a gluten-free diet trial, support immune regulation with low-dose naltrexone (LDN) under supervision if everything else you have tried isn’t helping, anti-inflammatory herbs like turmeric, or addressing infections
2. Impaired T4-to-T3 Conversion
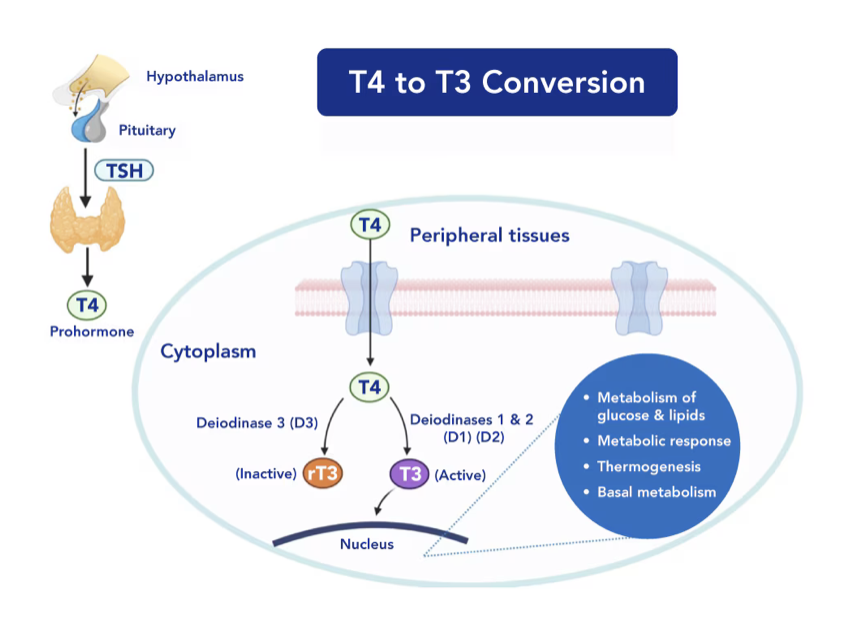
Levothyroxine (Synthroid) provides mostly inactive T4, which the body must convert to active T3 via deiodinase enzymes. This process is highly variable and inefficient in many thyroid patients.
There are three deiodinases—D1 and D2 activate T4 to T3 (in liver, kidneys, muscles, and gut), while D3 inactivates to reverse T3 (rT3), which blocks T3 receptors. Stress, inflammation, or deficiencies shift toward more rT3 production. Having muscle- meaning lifting weights to gain muscle and having a healthy gut can improve thyroid hormone conversion.
Why it fluctuates: Conversion depends on daily factors like calorie intake. You need to make sure you are eating enough because low-calorie diets impair conversion. Inflammation levels, liver function, and even time of day also affect conversion. Poor conversion means you might have "normal" labs but you still feel hypothyroid.
Key influencers: High cortisol or cytokines (from stress/infection) inhibit D1/D2; fasting or illness reduces it further. Take note of the health “experts” online telling you ladies to fast. If you have thyroid problems, fasting is the last thing you should be doing.
Conversion of T4 to T3 depends on many things including diet, liver health, and inflammation.
Root cause approach: Test free T3, free T4, and reverse T3 (optimal ratio >20). Optimize with selenium, zinc, and avoiding extreme dieting. Some benefit from adding T3 medication (like liothyronine or desiccated thyroid) if conversion remains poor. Test your mineral levels before supplementing.
3. Adrenal and Stress Axis Dysregulation
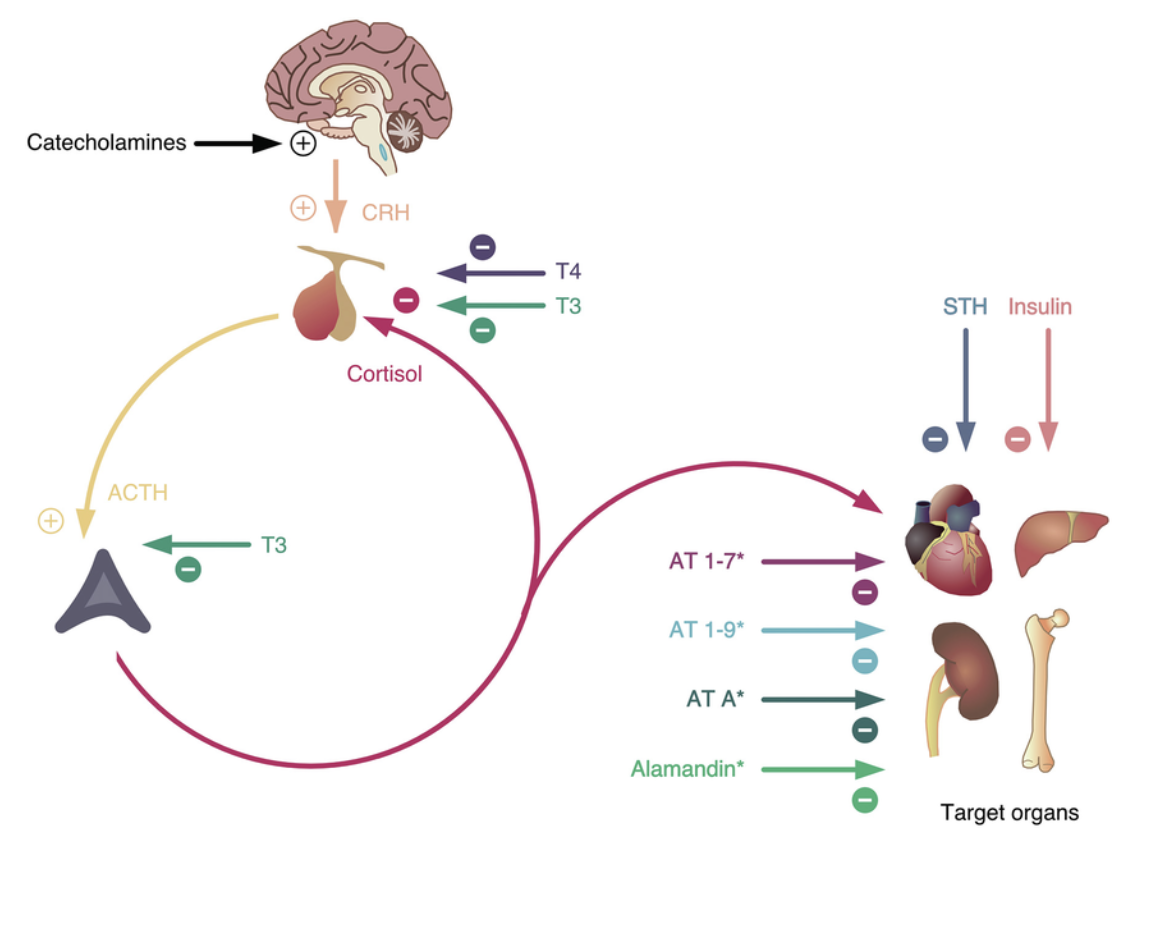
The thyroid and adrenals are tightly linked via the hypothalamic-pituitary-adrenal (HPA) axis, the body's stress response system.
Chronic stress signals the hypothalamus to release CRH, prompting pituitary ACTH and adrenal cortisol. Elevated cortisol suppresses TSH production, blocks T4-to-T3 conversion, and increases rT3. In later stages ("adrenal fatigue"), cortisol can drop too low, worsening fatigue and hormone signaling.
Stress is a big factor in adrenal and thyroid function.
Why symptoms fluctuate: Stress isn't constant—daily life (work, relationships, poor sleep) causes cortisol spikes or crashes, directly altering thyroid function hour-to-hour or day-to-day.
Common patterns: Worse symptoms in the morning (cortisol should peak) or during high-stress periods.
Root Cause approach: 4-point salivary or urine cortisol testing to map patterns. Support with adaptogens (ashwagandha, rhodiola), phosphorylated serine for high cortisol, B vitamins, magnesium, and stress reduction practices (breathwork, boundaries).
4. Gut and Microbiome Imbalances
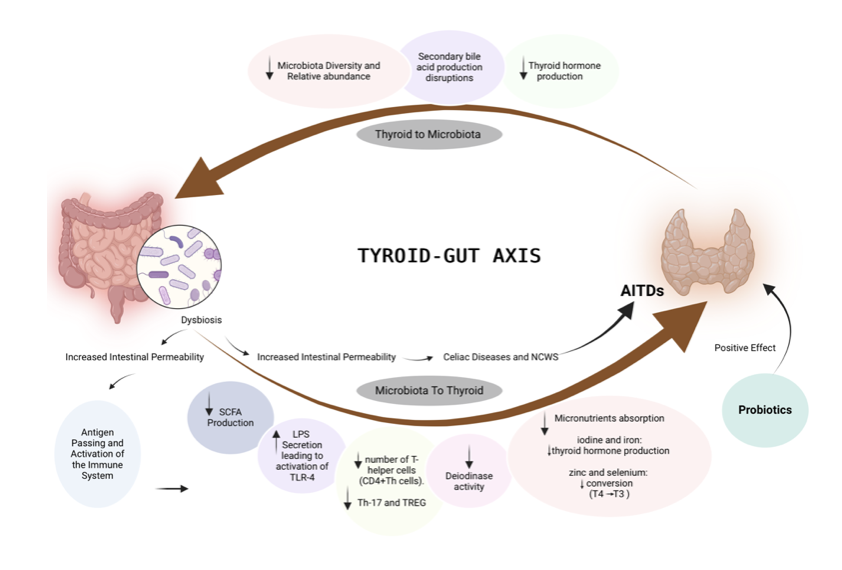
The gut is a major site of thyroid hormone activation and absorption, often called the "thyroid-gut axis."
About 20% of T4-to-T3 conversion occurs in the intestines via bacterial enzymes (e.g., sulfatases). Dysbiosis (imbalanced bacteria), SIBO, or leaky gut impairs this, reduces medication absorption, and allows toxins (LPS) to enter bloodstream, fueling systemic inflammation and autoimmunity.
Triggers for fluctuation: Dietary changes, antibiotics, infections, or stress alter the microbiome rapidly, shifting symptoms after meals or bowel changes.
dietary changes and infections rank among the most common and potent triggers for fluctuating thyroid symptoms, particularly in autoimmune cases like Hashimoto's. They often explain why symptoms can feel worse on certain days or after specific events, even when medication doses stay stable.
What you eat directly influences gut integrity, microbiome composition, inflammation levels, blood sugar stability, and immune tolerance. Changes—whether introducing trigger foods or removing them—can cause short-term shifts in thyroid function and symptoms
Inflammatory or Trigger Foods: Certain foods provoke immune responses or increase systemic inflammation, especially in sensitive individuals. Gluten stands out as a top offender due to molecular mimicry—its protein structure (gliadin) closely resembles thyroid tissue (thyroperoxidase enzyme). When the immune system attacks gluten, it can cross-react and attack the thyroid, spiking antibodies and causing a flare.
Other common triggers include dairy (casein mimicry), soy, eggs, nightshades, or grains. Processed foods high in sugar or refined carbs drive inflammation via advanced glycation end-products (AGEs) and disrupt the microbiome.
Blood Sugar Swings: High-glycemic meals (sugary or carb-heavy) cause insulin spikes followed by crashes, triggering cortisol release. Cortisol then suppresses TSH and blocks thyroid hormone activation. This creates daily or meal-to-meal variability—e.g., post-meal crashes worsening hypothyroid symptoms.
Positive Dietary Changes (e.g., Elimination Diets): Switching to an anti-inflammatory diet (gluten-free, dairy-free, Paleo, or AIP) often leads to long-term stability, but the transition can cause temporary fluctuations. Removing triggers reduces inflammation over time, but initial "die-off" (from shifting microbiome) or detox reactions can mimic worsening symptoms for days to weeks. Conversely, reintroducing a trigger during testing can confirm its role by reproducing symptoms.
Microbiome Shifts: Diet alters gut bacteria rapidly (within 24–48 hours). A poor diet promotes dysbiosis, reducing T3 conversion in the gut and increasing LPS (bacterial toxins) that fuel autoimmunity.
How fluctuations happen: Eating a trigger food (e.g., pizza with gluten and dairy) can increase gut permeability ("leaky gut") within hours, allowing undigested proteins into the bloodstream. This sparks inflammation, raises cytokines, and temporarily impairs T4-to-T3 conversion or boosts reverse T3. Symptoms like fatigue, brain fog, or joint pain may worsen for 1–3 days (or longer with repeated exposure).
Infections and Fluctuations
Infections—acute, chronic, or reactivating—powerfully trigger thyroid flares by activating the immune system and often through molecular mimicry, where pathogen proteins resemble thyroid proteins, leading to cross-reactivity.
Viral Infections: Epstein-Barr virus (EBV, cause of mono) links strongly to Hashimoto's. Many patients trace symptom onset to a past EBV infection; the virus can linger dormant and reactivate under stress, directly infecting thyroid cells or triggering antibodies.
Other viruses like CMV, HSV, or even recent ones (e.g., post-COVID thyroid issues reported) can do the same. Reactivation causes intermittent immune activation.
Bacterial and Gut Infections: Pathogens like H. pylori, Yersinia enterocolitica, or Borrelia (Lyme) use molecular mimicry. Gut-focused infections (SIBO, parasites, or dysbiosis from antibiotics) impair thyroid medication absorption and T3 conversion while leaking toxins that drive systemic inflammation.How fluctuations happen: An acute infection (flu, sinusitis) can spike inflammation broadly; chronic gut infections cause ongoing variability tied to digestion or die-off during treatment.
How fluctuations happen: During a flare (e.g., from stress or another illness), rising viral antibodies cross-react with thyroid tissue, causing inflammation and erratic hormone release. Symptoms may intensify for weeks, then subside until the next trigger.
From a functional medicine viewpoint, these triggers disrupt the delicate balance of the immune system, gut, hormone conversion, and inflammation—leading to episodic "flares" rather than constant issues.
These triggers are inherently episodic—a single triggering meal or a stress-induced viral reactivation can shift symptoms noticeably, explaining the "good days and bad days" pattern.
Functional approach: Test for chronic infections (EBV/EBNA/VCA antibodies, stool tests for pathogens, or organic acids urine test).
Support with antimicrobials (herbs like oregano oil, berberine under guidance), immune modulation, and addressing triggers to prevent recurrences.
Diet and infections often interplay (e.g., poor diet weakens immunity, increasing infection risk). Many patients see more consistent symptoms once these are addressed.
Links to autoimmunity: Low bacterial diversity is common in Hashimoto's; certain pathogens trigger molecular mimicry.
Functional approach: Comprehensive stool testing (e.g., GI-MAP). Heal with probiotics, prebiotics, L-glutamine, bone broth, and eliminating triggers (gluten, dairy often cross-react).
5. Nutrient Deficiencies and Toxin Exposure
Thyroid function relies on specific nutrients for hormone synthesis, conversion, and protection, while toxins disrupt these processes.
Key nutrients:
Selenium protects thyroid from oxidative damage and supports deiodinases.
Iron/ferritin for thyroid peroxidase enzyme.
Zinc for T3 receptor function.
Vitamin D modulates immunity.
Deficiencies fluctuate with diet, absorption issues, or increased needs during stress.
Toxins: Heavy metals (mercury), mold mycotoxins, BPA/plastics, or halides (fluoride) compete with iodine or burden liver detox, causing variable interference.
Why fluctuating: Seasonal diet changes, exposure variations (e.g., mold in damp weather), or poor gut absorption lead to ups and downs.
Root Cause approach: Comprehensive nutrient testing (serum + intracellular if possible). Replete gradually (e.g., Brazil nuts for selenium). Detox support with sauna, binders (charcoal, clay), and liver herbs (milk thistle).
6. Hormonal Interplay (Sex Hormones, Blood Sugar)
Thyroid hormones interact with estrogen, progesterone, insulin, and cortisol.
Sex hormones: Estrogen (higher in luteal phase or perimenopause) increases thyroid-binding globulin (TBG), binding more T4/T3 and reducing free (active) levels. Progesterone supports thyroid utilization.
Blood sugar: Insulin resistance or hypoglycemia triggers cortisol release, impairing conversion. Meals high in refined carbs cause swings.
Why fluctuating: Cyclical (menstrual cycle, perimenopause) or meal-related changes drive daily/weekly shifts—e.g., worse fatigue mid-cycle or post-meal crashes.
Functional approach: Test sex hormones (Dutch test for metabolites), stabilize blood sugar (low-glycemic diet, chromium, berberine). Balance estrogen with DIM/broccoli sprouts or progesterone support if needed.
These interconnections explain why symptoms feel like a moving target. Addressing multiple layers often brings more stability than medication adjustments alone. Tracking patterns in a journal can reveal your personal triggers.
Schedule a call with me to get to your root cause and start feeling well again.
Detox Toxins for Thyroid Health
If you’re dealing with thyroid issues like Hashimoto’s or Graves’, toxins in your environment might be making things worse. As a certified nutrition specialist and licensed nutritionist, I’m here to explain how toxins affect your thyroid and how digestion helps detox them. Let’s explore simple ways to reduce toxins and support your thyroid, based on nutritional therapy principles.
Toxins and Your Thyroid
Environmental toxins like BPA, phthalates, and PFAS (from plastics, cans, or receipts) can disrupt thyroid hormones, increasing inflammation and worsening symptoms like fatigue or weight gain. A 2019 study found home-cooked meals lower PFAS levels by 5%. Your digestive system, especially bile and stool, helps remove these toxins.
How Digestion Detoxifies
Your liver and gallbladder produce bile, which binds toxins in the small intestine for removal through stool. Poor digestion, like low bile flow or constipation, traps toxins, stressing your thyroid. For example, trapped toxins might raise estrogen, interfering with thyroid function.
Toxins and Inflammation
Toxins increase inflammation, which can trigger autoimmune flares in Hashimoto’s. They also disrupt gut bacteria, reducing nutrient absorption like selenium, worsening thyroid symptoms.
Common Toxin Sources
Toxins sneak in from:
Plastics: BPA in containers or water bottles.
Canned Foods: Contain PFAS or BPA.
Receipts: Transfer toxins to your skin.
These can accumulate, stressing your thyroid.
Practical Tips for Thyroid-Friendly Detox
Here are easy ways to reduce toxins and support your thyroid, fitting your love for home-cooked meals:
Use Glass Containers: Store food in glass or stainless steel.
Avoid Canned Foods: Choose fresh or frozen veggies.
Wash Hands: After handling receipts to reduce toxin exposure.
Eat Detox Foods: Try broccoli or kale to support liver detox.
Stay Hydrated: Drink 8 glasses of water to aid toxin removal.
Try Supplements: N-acetylcysteine (NAC) or milk thistle for detox at www.outofthewoodsnutrition.com/dispensary (consult your doctor).
Why It Helps
Reducing toxins and supporting digestion lowers inflammation, balances hormones, and fuels your thyroid, easing symptoms like brain fog.
Work With Your Doctor
I don’t diagnose, but I can guide you with diet and lifestyle. Work with your healthcare provider to monitor thyroid levels and discuss toxin exposure.
Take Action
Swap one plastic container for glass this week. Book a consultation at www.outofthewoodsnutrition.com. Visit www.outofthewoodsnutrition.com/dispensary.
What’s your favorite detox food? Comment below!
About the Author: I’m a certified nutrition specialist and licensed nutritionist, helping women with thyroid conditions feel vibrant. Visit www.outofthewoodsnutrition.com for more tips.